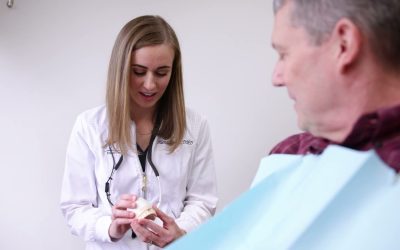
If you’re experiencing jaw pain, clicking sounds, or headaches and have scheduled a TMJ consultation in Itasca, you might be wondering exactly what the appointment will involve. The process is designed to be thorough and educational, focusing on identifying the root cause of your discomfort rather than just treating symptoms. For residents of Itasca, Wood Dale, and the surrounding DuPage County area, understanding this step-by-step approach can help demystify the experience and prepare you for a productive partnership with your dental provider.
Table of Contents
Key Takeaways | Before Your Appointment | Step 1: Health History | Step 2: Clinical Exam | Step 3: Bite & Imaging | Step 4: Findings & Plan | Local Insight | FAQs
Key Takeaways (TL;DR)
- A collaborative conversation: The consultation starts with a detailed review of your symptoms, health history, and daily habits—your input is crucial for an accurate diagnosis.
- Hands-on assessment: The dentist will physically examine your jaw joints, muscles, and bite, measuring range of motion and listening for sounds.
- Technology for clarity: Advanced tools like digital bite analysis or CBCT scans may be used to visualize joint structure and function, providing objective data.
- Clear pathway forward: The goal is to leave with a clear understanding of your diagnosis and a personalized, conservative treatment plan tailored to your specific needs.
Preparation: What to Bring and Note Before Your Itasca Appointment
Being prepared helps ensure your consultation is as efficient and informative as possible. Taking a few moments before your visit can provide your Itasca dentist with valuable context about your symptoms and lifestyle.
What to Bring to Your TMJ Consultation
- Medical History: A list of current medications, supplements, and any relevant medical conditions (e.g., arthritis, sleep disorders, chronic pain conditions).
- Dental History: Previous X-rays or imaging, especially if you’ve had them taken elsewhere. Information about past dental work, orthodontics, or trauma to the face or jaw.
- Insurance Information: Your dental and medical insurance cards, as coverage for TMJ diagnostics can vary between plans.
What to Note Before You Arrive
In the days leading up to your appointment, consider keeping a simple symptom log. This doesn’t need to be complex, but noting the following can be incredibly helpful:
This preparation transforms you from a passive patient into an active participant in your diagnosis, leading to a more targeted and effective consultation at your Itasca dental practice.
Step 1: The Comprehensive Health and Symptom History Review
The consultation begins with conversation, not examination. This detailed discussion is arguably the most critical part of the process, as it provides context that guides the entire physical assessment. Your dentist in Itasca will listen carefully to understand your unique experience.
Key Areas of Discussion
Be prepared to discuss the following in detail. Dentists trained in TMJ evaluation are looking for patterns and connections:
- Symptom Onset & Pattern: When did the pain or clicking start? Was it sudden or gradual? Is it constant or intermittent?
- Pain Description: The exact location (jaw joint, temples, ears, neck), type (dull ache, sharp pain, pressure), and intensity (often rated on a 0-10 scale).
- Function & Habits: Does it hurt to chew, talk, or yawn? Are you aware of clenching, grinding (bruxism), or nail-biting? Do you chew gum frequently or have other oral habits?
- Lifestyle & Medical Factors: Stress levels, sleep quality (including snoring or witnessed apnea), diet, posture at work, history of jaw injury, and any related conditions like arthritis or fibromyalgia.
- Impact on Daily Life: How are symptoms affecting your work, sleep, diet, and overall quality of life?
This collaborative dialogue sets the stage for a focused physical examination. Your detailed account allows the dentist to test specific hypotheses during the hands-on assessment that follows.
Step 2: The Clinical Examination of Jaw Joints and Muscles
Following the detailed history, the dentist will perform a hands-on clinical examination. This step objectively assesses what was discussed, measuring function, identifying tender areas, and evaluating the health of your jaw’s structures. For patients in Itasca and Addison, this exam is typically painless and informative.
Visual and Palpation Assessment
The dentist will first look for visual signs like facial symmetry, muscle bulk, and wear patterns on your teeth. Then, using their fingertips, they will gently palpate (press on) specific areas:
- Jaw Joints (TMJs): Just in front of your ears to feel for tenderness, swelling, or vibration during movement.
- Chewing Muscles: The masseter (cheek) and temporalis (temple) muscles are checked for tightness, trigger points, and pain.
- Neck and Shoulder Muscles: Because posture plays a significant role, muscles in the neck and upper back are often assessed for contributing tension.
Measuring Jaw Range of Motion and Sounds
This part quantifies your jaw’s function. The dentist may use a small ruler or caliper to measure, in millimeters:
- Maximum Unassisted Opening: How wide you can open your mouth comfortably. (Normal range is typically 35-55mm).
- Maximum Assisted Opening: How wide you can open with gentle help, testing for muscle vs. joint restrictions.
- Side-to-Side and Forward Movements: Assessing lateral mobility and protrusion.
They will also listen and feel for clicking, popping, or grating sounds (crepitus) during these movements, which can indicate disc displacement or joint surface changes.
Opening
35-55mm typical
Side Shift
Assesses joint glide
Palpation
Checking for tenderness
The data gathered from this examination creates a functional baseline and helps correlate your subjective symptoms with objective clinical signs, guiding the next steps in diagnosis.
Step 3: Bite Analysis and Advanced Diagnostic Imaging (If Needed)
This step moves from external assessment to analyzing the interface between your teeth and the internal structure of the joints.
Bite (Occlusal) Analysis
The dentist will examine how your teeth fit together. They look for:
- Wear Facets: Flat, shiny spots on teeth indicating grinding.
- Malocclusion: Misalignment that may force the jaw into a strained position.
- Muscle Recruitment Patterns: Which muscles engage when you bite down.
They may take a bite registration using a soft material to record your jaw’s position.
Advanced Imaging
Not all cases require advanced imaging. It is typically recommended if:
- The history or exam suggests joint pathology (arthritis, severe disc displacement).
- Symptoms are severe, persistent, or involve trauma.
- Surgical intervention is being considered.
This phase provides the concrete anatomical data needed to finalize a precise diagnosis and formulate an effective treatment plan.
Step 4: Reviewing Findings and Discussing Your Personalized Plan
After gathering all diagnostic information, the dentist will synthesize the findings with you. This collaborative review ensures you understand the “why” behind your symptoms and the “how” of the proposed solution.
The Diagnosis and Explanation
You will receive a clear diagnosis, which may fall into categories such as:
- Myofascial Pain: Primary issue is muscle tension and trigger points.
- Internal Derangement: Problem with the joint’s disc (e.g., displacement).
- Degenerative Joint Disease: Arthritis affecting the joint surfaces.
- Combination Disorder: Mix of muscular and joint issues.
The dentist will explain how your specific symptoms, exam findings, and any imaging correlate to this diagnosis.
The Treatment Pathway Discussion
Based on the diagnosis, the dentist will outline a conservative, phased treatment plan. This is not a one-size-fits-all prescription but a tailored strategy. Key components often include:
Home instructions, habit modification, diet changes.
Custom oral appliance, physical therapy referral.
Follow-up to assess progress and adjust the plan.
The discussion will cover:
- Realistic Expectations: Timeline for improvement and treatment goals.
- Financial Considerations: Cost estimates and a review of potential insurance coverage.
- Next Steps: Scheduling for appliance fabrication, physical therapy evaluation, or a follow-up visit.
Local Insight: The Itasca Approach to Collaborative Diagnosis
In Itasca and the broader DuPage County dental community, the standard of care for TMJ disorders emphasizes a coordinated, patient-centered model. Modern practices here are equipped not just to diagnose but to connect findings to a network of local health resources.
Integrated Care Networks
Many dental providers in the area have established referral relationships with trusted local specialists. If your consultation indicates a need for focused care beyond the dental scope, your dentist can facilitate a seamless connection:
- Physical Therapists: For targeted jaw and cervical spine rehabilitation; practices in Roselle, Elmhurst, and Medinah often specialize in TMJ.
- Sleep Medicine Physicians: If symptoms strongly suggest sleep apnea, a referral for a formal sleep study can be coordinated.
- Oral & Maxillofacial Surgeons: For advanced surgical evaluation, available at major surgical centers in the region.
Emphasis on Patient Education and Empowerment
Consistent feedback from patients in Wood Dale, Addison, and Schaumburg highlights the value placed on understanding their condition. Local dentists invest time in explaining:
- The biomechanics of their specific jaw issue.
- How daily habits (commute posture, work stress) contribute.
- The “why” behind each recommended therapy.
This local model of care ensures that while your journey might begin in a general dental chair in Itasca, the pathway to comprehensive management—whether it involves muscle relaxation, joint stabilization, or airway health—is clearly mapped and supported by a community of professionals.
Frequently Asked Questions About TMJ Consultations
Patients in Itasca often have specific, practical questions about what to expect. Here are answers to some of the most common queries.
How long does a TMJ consultation take in Itasca?
Plan for approximately 60 to 90 minutes. A thorough consultation requires time for a detailed conversation, clinical examination, and discussion of findings. Rushed appointments often miss critical details, so quality practices in DuPage County allocate sufficient time.
Is the clinical examination painful?
The examination should not be painful, but it may provoke some familiar discomfort. When palpating tender muscles or joints, you may feel pressure or a reproduction of your usual ache. It’s important to communicate what you’re feeling to your dentist, as this feedback is part of the diagnostic process.
Will I get a diagnosis and treatment plan in the first visit?
In most cases, yes. The goal of a comprehensive consultation is to provide you with a working diagnosis and a preliminary treatment plan before you leave. If advanced imaging is required and wasn’t done previously, a definitive diagnosis might be confirmed at a brief follow-up after reviewing the images.
What if my dental or medical insurance doesn’t cover the consultation?
Coverage varies widely. Many Itasca-area dental practices will verify your benefits beforehand and discuss out-of-pocket costs transparently prior to your appointment. Some diagnostic codes may fall under medical insurance if a related medical condition (like sleep apnea) is being evaluated. Always ask the office staff for a benefits check and cost estimate.
People Also Search For
- TMJ specialist vs general dentist Itasca
- What to wear to a TMJ appointment
- Cost of TMJ evaluation without insurance Itasca
- Questions to ask your dentist about jaw pain
Next Step: Understanding the diagnostic process is the first step toward addressing jaw pain. For a deeper look at the treatment options that may follow a consultation, explore our overview of TMJ disorders and available treatments in Itasca.
Sources & References
This guide is based on current standards of care and authoritative sources in orofacial pain and dental diagnosis.
- American Academy of Orofacial Pain (AAOP). Guidelines for Assessment, Diagnosis, and Management of Orofacial Pain.
- The National Institute of Dental and Craniofacial Research (NIDCR). “Temporomandibular Disorders.”
- Journal of Oral & Facial Pain and Headache. Peer-reviewed literature on TMJ diagnostic criteria and protocols.
- American Dental Association (ADA). Council on Scientific Affairs reports on temporomandibular disorders.
Last reviewed: December 2025
About the Dentist & Practice
Dr. Kathy French and the team at Hamilton Lakes Dentistry provide comprehensive dental care, including detailed TMJ consultations, to the Itasca community and surrounding DuPage County areas. The practice emphasizes patient education, thorough diagnosis, and collaborative treatment planning for conditions affecting the jaw joint and orofacial complex.
Located at 500 Park Blvd #180c in the Hamilton Lakes Business Park, the practice serves patients from Itasca, Wood Dale, Addison, Bloomingdale, and Schaumburg. For more information about their approach to TMJ and overall dental health, you can meet the team here.